Understanding Malabsorption and Nutrient Deficiency in Dogs
- Apr 3
- 11 min read
Updated: May 17
About 60% of dogs with exocrine pancreatic insufficiency (EPI) improve well on enzyme replacement therapy – yet about half of dogs with protein‑losing enteropathy (PLE) die within 12 months of diagnosis.[6][8] Same body system, same broad problem (poor nutrient absorption), completely different outcomes.
That contrast is at the heart of malabsorption in dogs: it often looks similar on the surface – weight loss, dull coat, diarrhea – but the biology underneath can range from very manageable to genuinely life‑limiting. When a dog keeps losing weight despite eating, or their coat looks lifeless no matter what food you buy, it isn’t about you “failing” them. It’s often about their gut simply not doing its job.

This article is here to unpack that job – how nutrient absorption is supposed to work, what happens when it doesn’t, what those symptoms are really telling you, and how to think clearly about next steps with your vet.
What “malabsorption” actually means
Malabsorption isn’t a single disease. It’s a description: your dog’s small intestine is not absorbing nutrients properly.

That failure can come from several directions:
the food isn’t broken down enough to be absorbed (maldigestion)
the intestinal lining is damaged or inflamed
the lymphatic “drainage” system in the gut is blocked or leaky
abnormal bacteria are interfering with digestion
specific nutrients simply can’t cross the intestinal wall
Key terms you’ll hear
You’ll likely meet some of these phrases in vet conversations:
Malabsorption: Poor absorption of nutrients in the small intestine. A result, not a diagnosis.
Exocrine Pancreatic Insufficiency (EPI): The pancreas doesn’t produce enough digestive enzymes (protease for protein, lipase for fat, amylase for starch). Food isn’t properly broken down, so even excellent diets pass through largely unused.
Inflammatory Bowel Disease (IBD): Chronic inflammation of the gastrointestinal tract. The immune system is overactive in the gut lining, damaging the mucosa and reducing absorption.
Small Intestinal Bacterial Overgrowth (SIBO) / Dysbiosis: Too many or the wrong kinds of bacteria in the small intestine. They consume nutrients, produce irritating by‑products, and disrupt normal digestion.
Protein‑Losing Enteropathy (PLE): The gut is losing important blood proteins (especially albumin) into the intestinal lumen. This causes low blood protein, swelling, and often serious malnutrition.
Villous atrophy: The finger‑like projections (villi) that increase the intestine’s surface area become shortened or damaged, so there’s simply less “absorbing surface” to work with.
Selective cobalamin (vitamin B12) malabsorption: A specific failure to absorb B12 from the intestine, often inherited in certain breeds (notably Giant Schnauzers), leading to anemia and failure to thrive.
All of these can end in the same place:
a dog who’s eating, but not really “getting fed.”
How malabsorption shows up in real life
Different causes of malabsorption have their own patterns, but there’s a shared cluster of signs that often overlap.

Common symptoms of malabsorption and nutrient deficiency
Weight loss despite normal – or increased – appetite
Chronic diarrhea or persistently loose stools
Pica (eating non‑food items like soil, wood, fabric)
Lethargy, low energy, or “slowed down” behavior
Poor coat quality: dull, dry, brittle, or thinning
Flatulence and bloating
Vomiting (occasional or frequent)
Muscle wasting or weakness
In severe PLE: fluid accumulation (swollen belly, limb swelling), because of low blood protein

Owners often describe a particular contradiction:
“My dog is ravenous, but keeps getting thinner.”
That paradox is a major red flag for EPI and other malabsorption problems.
Breeds, genetics, and “why my dog?”
Any dog can develop malabsorption, but some patterns are well documented:
German Shepherds: Predisposed to EPI, small intestinal bacterial overgrowth, and PLE.[3][6][7]
Yorkshire Terriers: Over‑represented in intestinal lymphangiectasia (a form of PLE where intestinal lymph vessels leak protein).[3]
Sled dogs (Alaskan Malamute, Siberian Husky): Known for genetic zinc malabsorption issues, which can show as skin disease and poor coat.[5]
Giant Schnauzers: Reported to have inherited selective intestinal cobalamin (B12) malabsorption with an autosomal recessive pattern.[4]
Genetics doesn’t mean inevitability, but if your dog is in one of these groups, it can sharpen your vet’s suspicion and speed up diagnosis.
What’s going wrong inside: main causes of malabsorption
You don’t need to become a gastroenterologist, but having a mental map of the main categories helps you ask better questions and understand your vet’s plan.
1. Exocrine Pancreatic Insufficiency (EPI)
Core problem: not enough digestive enzymes.
Without adequate enzymes, fats, proteins, and carbohydrates aren’t properly broken down. Large, poorly digested molecules move into the intestine, drawing water in (diarrhea), feeding bacteria, and exiting largely unused.
Typical picture:
marked weight loss despite a big appetite
voluminous, often pale or greasy stools
flatulence
poor coat condition
sometimes pica

Treatment outlook: Enzyme replacement therapy is usually lifelong but often very effective. In one study, about 60% of dogs with EPI responded well to enzyme replacement, and another 17% showed partial improvement.[6][8] Many dogs with EPI can live good, active lives once dosing and diet are stabilized.
2. Inflammatory Bowel Disease (IBD)
Core problem: chronic inflammation of the gut wall.
The immune system is over‑responding in the intestines, damaging the mucosa and causing:
reduced absorption surface
leaky barriers
pain, diarrhea, and sometimes vomiting
IBD often overlaps with food sensitivities, microbiome changes, and immune dysregulation. It’s one of the classic chronic causes of malabsorption.

Management usually includes:
carefully chosen diets (novel protein, hydrolyzed, or highly digestible)
immunosuppressive or immunomodulatory drugs
sometimes antibiotics for concurrent dysbiosis
A retrospective study of 17 dogs with malabsorption syndrome found that combined dietary and immunosuppressive treatment improved clinical condition, body weight, and serum protein levels.[2]
That’s a small sample, but it echoes what many internists see in practice: you often need to treat both the immune system and the diet.
3. Protein‑Losing Enteropathy (PLE)
Core problem: the intestine is leaking blood proteins into the gut.
This can come from:
intestinal lymphangiectasia (damaged lymph vessels)
severe IBD
intestinal cancers
other structural diseases of the gut
Because albumin and other proteins are lost, dogs can develop:
fluid accumulation (belly, limbs, chest)
weight loss and muscle wasting
diarrhea
sometimes blood clots, because protein loss affects clotting factors
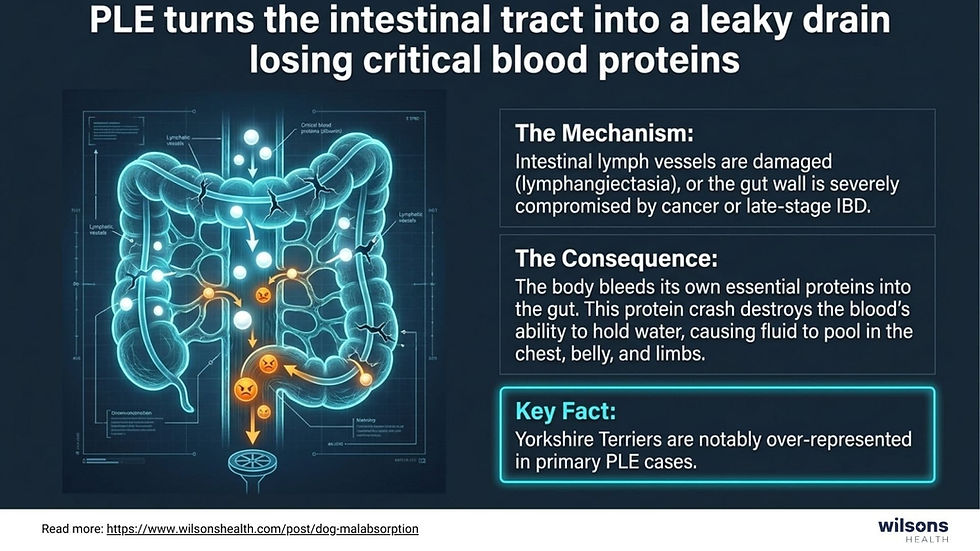
Prognosis: PLE is one of the more serious outcomes of chronic intestinal disease. Reported data suggest that over 50% of dogs with PLE die within 12 months of diagnosis, despite treatment.[6][8] Some dogs respond very well to diet plus immunosuppression; others do not. This is where early diagnosis and honest expectation‑setting become very important.
4. Small Intestinal Bacterial Overgrowth (SIBO) / Dysbiosis
Core problem: too many – or the wrong – bacteria in the small intestine.
These bacteria:
compete with your dog for nutrients
deconjugate bile acids (disrupting fat digestion)
produce toxins and gas
inflame or damage the mucosa
This can occur on its own, but often it’s secondary to something else (like EPI or IBD). That’s why treating dysbiosis alone may not fully solve the problem if the root cause is still there.[6][7]

5. Specific nutrient malabsorption
Sometimes the issue is not global absorption, but a particular nutrient:
Cobalamin (vitamin B12): Essential for red blood cell production and nervous system function. Inherited selective cobalamin malabsorption in breeds like Giant Schnauzers leads to failure to thrive and anemia.[4] Many dogs with chronic small intestinal disease also develop secondary B12 deficiency because the part of the gut that absorbs B12 is inflamed or damaged.
Zinc: Certain northern breeds can have genetic problems with zinc absorption, leading to skin disease, poor coat, and sometimes immune issues.[5]
These cases often respond well to targeted supplementation (e.g., B12 injections, zinc), but they still require a proper diagnosis – giving random supplements without understanding the underlying issue can obscure what’s really happening.
How vets figure it out: from “my dog’s too thin” to a diagnosis
Because “weight loss and diarrhea” can mean many things, malabsorption work‑ups are often stepwise. Your vet isn’t trying random tests; they’re narrowing down a long list.

Typical diagnostic tools
History and physical exam: Duration of symptoms, appetite changes, stool description, weight trends, breed, travel history, diet changes. Your observations of pica, coat quality, or subtle personality changes often provide crucial clues.[1][13]
Basic lab work:
Complete blood count (CBC)
Biochemistry profile (including proteins, liver, kidney values)
Electrolytes
Low albumin may suggest PLE; anemia may point toward chronic disease or B12 deficiency.
Fecal exams: To rule out parasites and some infectious causes.
Specific blood tests:
Trypsin‑like immunoreactivity (TLI) to diagnose EPI
Cobalamin (B12) and folate levels as markers of absorption and bacterial overgrowth
Sometimes inflammatory markers
Imaging: Abdominal ultrasound to assess intestinal thickness, lymph nodes, lymphatic vessels, and other organs.
Endoscopy and biopsy: A camera is passed into the stomach and small intestine to take tissue samples. This is the gold standard for diagnosing IBD, intestinal lymphangiectasia, and some cancers.[3][10]
None of these tests alone is “the malabsorption test.” Instead, they build a picture of why your dog is not absorbing nutrients.
Treatment isn’t one thing – it’s a toolkit
There is no single “malabsorption diet” or “malabsorption pill.” Management depends on the underlying cause, but the tools tend to fall into a few categories.

Dietary management
Food is both trigger and therapy in many intestinal diseases.
Common strategies include:
High‑digestibility diets: To reduce the workload on a compromised gut.
Novel protein or hydrolyzed diets: For suspected food‑responsive disease or IBD, reducing immune activation in the gut.
Low‑fat diets: Particularly important for intestinal lymphangiectasia and some PLE cases, to reduce lymph flow and protein loss.
Careful treat management: Seemingly small extras can derail otherwise well‑controlled disease.
A retrospective study of dogs with malabsorption showed that dietary changes combined with immunosuppressive drugs improved weight and serum proteins.[2]
Diet alone sometimes helps; diet plus targeted medication often helps more.
Enzyme and nutrient supplementation
Pancreatic enzyme replacement for EPIUsually a lifelong addition to each meal. Getting the dose and form right can be a bit of an early balancing act.
Cobalamin (B12) injections or oral supplementation: For dogs with low B12, whether from genetic causes or secondary to chronic intestinal disease.
Other targeted nutrients: Such as zinc in predisposed breeds, or specific amino acids in severe protein loss – always under veterinary guidance.
Medications
Depending on the diagnosis, your vet may recommend:
Immunosuppressive drugs: Such as corticosteroids or other agents to control IBD or immune‑mediated PLE.
Antibiotics or microbiome‑directed therapies: For bacterial overgrowth/dysbiosis, often as part of a broader plan.
Anti‑diarrheal or anti‑nausea medications: To improve comfort while the underlying issue is addressed.
Because many of these treatments are long‑term, the conversation around risks, benefits, and monitoring should be ongoing and open. There is rarely a “perfect” option, only the best‑fitting one for your dog and your household at that time.
Monitoring
Chronic intestinal disease is rarely a “treat for 10 days and forget it” situation. Ongoing monitoring typically involves:
regular weight checks (home and/or clinic)
body condition and muscle condition scoring
stool quality tracking
periodic blood tests (proteins, B12, general health)
watching for side effects of medications
Think of it as managing a long‑term condition like arthritis or diabetes, but in the gut.
Prognosis: why some dogs bounce back and others don’t
The word “malabsorption” doesn’t tell you the outlook; the cause does.

A broad, simplified comparison:
Condition | Typical Prognosis with Treatment |
EPI | Often good to excellent; many dogs live full lives on enzymes.[6][8] |
Mild–moderate IBD | Fair to good; many respond to diet ± immunosuppression. |
Severe IBD with PLE | Guarded; response variable, some long‑term successes, some not. |
Primary PLE (e.g., lymphangiectasia) | Guarded to poor; >50% mortality within 12 months reported.[6][8] |
Inherited B12 malabsorption | Variable; can be managed if recognized and supplemented early.[4] |
These aren’t predictions for your individual dog; they’re population‑level patterns. They are, however, useful for framing expectations:
Some conditions are manageable but not curable (EPI, many IBD cases).
Some are serious and time‑sensitive, where early intervention can make a meaningful difference (PLE).
Some may remain somewhat mysterious, even after extensive testing, because gut disease is genuinely complex.
The emotional side: when feeding your dog becomes a source of worry
Living with a dog who has malabsorption is not just a medical project; it’s an emotional one.

Common experiences owners describe:
Guilt – “He’s so thin. I must be doing something wrong.”In reality, many of these conditions have nothing to do with feeding choices. You didn’t cause your dog’s pancreas to fail or their villi to atrophy.
Frustration and confusion – “I changed foods, added supplements, nothing is working.”Because the problem is often inside the gut wall or pancreas, no over‑the‑counter change can fully fix it.
Chronic stress – managing special diets, medications, frequent vet visits, and unpredictable flare‑ups.
Financial worry – long‑term enzyme therapy, immunosuppressants, and diagnostics add up.
These feelings are not a sign you’re failing your dog; they’re a sign you care and you’re living with a chronic condition. Caregiver fatigue is real, even when the patient has four legs.
It’s completely reasonable to:
ask your vet to clarify priorities (“What are the must‑do things, and what’s optional?”)
discuss quality‑of‑life openly, not just lab values
set boundaries around what is sustainable for you and your family
Ethically, chronic GI disease often sits at the crossroads of what is medically possible and what is emotionally and financially sustainable. There is no single “right answer”; there is the best possible path for your particular dog, with your particular resources and values.
How to talk with your vet – and what to ask
You don’t need to arrive with a diagnosis; you can arrive with good questions.

Some conversation starters and clarifiers:
“Are we dealing mostly with digestion (like EPI), absorption (like IBD/PLE), or both?” This helps you understand whether the main problem is enzyme production, the gut lining, or something else.
“Which tests are most important to do first, and what decisions will they change?” Useful when you’re trying to prioritize within a budget.
“If this turns out to be chronic, what does long‑term management usually look like?” You’re asking for a rough roadmap, not a guarantee.
“What signs at home should make me call you right away?” For example: sudden swelling, severe lethargy, blood in stool, collapse.
“How will we monitor whether the treatment is working – weight, labs, stool, energy?” Having clear markers prevents you from feeling lost in the process.
“If my dog doesn’t respond as expected, what would the next step be?” It’s calming to know there’s a Plan B (and sometimes Plan C).
A good vet will welcome these questions. They signal that you want to be an informed partner, not that you’re doubting their expertise.
What is well‑known – and what isn’t (yet)
Veterinary medicine knows a lot about malabsorption, and also runs into genuine uncertainty.
Fairly well‑established
Causes like EPI, IBD, SIBO/dysbiosis, and PLE are clearly linked to malabsorption and nutrient deficiencies.[3][6][7]
Diagnostic methods like blood tests (TLI, B12), imaging, and especially endoscopic biopsies are effective for defining many underlying diseases.[3][10]
Treatments such as enzyme replacement for EPI and combined diet/immunosuppressive therapy for many IBD/PLE cases can significantly improve symptoms and lab values.[2][6]
Owner emotional impact is high; chronic GI disease reliably creates stress, worry, and caregiver burden.[1][7]
Still uncertain or emerging
The full role of the microbiome and dysbiosis – which changes are cause, which are effect, and how best to correct them.[6]
The optimal long‑term immunosuppressive protocols for IBD and PLE – balancing disease control with safety.
The detailed genetic mechanisms behind breed predispositions.
The best ways to provide emotional and practical support to owners beyond the strictly medical plan.
You may hear your vet say “we don’t fully know yet” about some aspect of your dog’s condition. That isn’t a failure; it’s honesty. In a system as complex as the gut, some uncertainty is built in.
Living with a dog who doesn’t absorb nutrients well
Once the initial crisis is over and a diagnosis (or at least a working diagnosis) is in place, life settles into a new rhythm.

Day‑to‑day, that often looks like:
measuring enzymes or medications into each meal
sticking to a carefully chosen diet and being “that person” who says no to well‑meaning treats from others
keeping a quiet eye on weight, stool, and energy levels
scheduling periodic blood tests and check‑ins
learning where your dog’s “wobble points” are – stress, diet slips, or other illnesses that can trigger flares
Over time, many owners become extremely attuned to their dog’s gut health. That knowledge is powerful. You start to see patterns, catch changes early, and advocate effectively for adjustments.
And perhaps most importantly: you see that your dog is not just a diagnosis. They are still themselves – still wanting walks, cuddles, games, sun‑patch naps – even if their intestine is a bit high‑maintenance.
Understanding the biology behind their symptoms doesn’t take away the hard parts, but it does something quieter and essential: it turns random fear into informed vigilance. You know what you’re watching for. You know what questions to ask. You know that “not gaining weight” has a name, a physiology, and, in many cases, a plan.
That clarity is its own kind of comfort.
References
What Causes Malabsorption in Dogs? - My Pet Nutritionist.
German AJ, Hall EJ, Day MJ. Pharmacological and dietary treatment of canine malabsorption syndrome: a retrospective study of 17 clinical cases. J Small Anim Pract.
Malabsorption in Dogs – Vetlexicon.
Fyfe JC et al. Inherited Selective Intestinal Cobalamin Malabsorption in Dogs. Nature.
Lack of Absorption of Nutrients in Dogs – Wag!.
Malabsorption Syndromes in Small Animals – MSD Veterinary Manual.
Malabsorption and Bacterial Overgrowth in Dogs – VCA Animal Hospitals.
Malabsorption Syndromes in Small Animals – Merck Veterinary Manual.
Intestinal Malabsorption in Dogs – WagWalking.
Hall EJ. Diagnosis and management of malabsorption in dogs. Wiley Online Library.
EPI in Dogs – And Other Digestive Diseases – Dogs Naturally.
Small Intestinal Malabsorption – Westwood Regional Veterinary Hospital.
Nutritional Deficiency In Dogs: Signs, Symptoms, and Solutions – Protexin Pet.
3 Sneaky Signs of Nutrient Deficiency in Dogs – Carnos.






Comments