When to Seek Professional Help for Dog Wounds
- Apr 22
- 10 min read
Updated: May 20
About 80–90% of dog wounds seen in general practice are not life-threatening, yet a surprisingly large number of complications come from one simple problem: owners waited too long to call the vet, assuming it was “just a scratch” that would heal on its own.
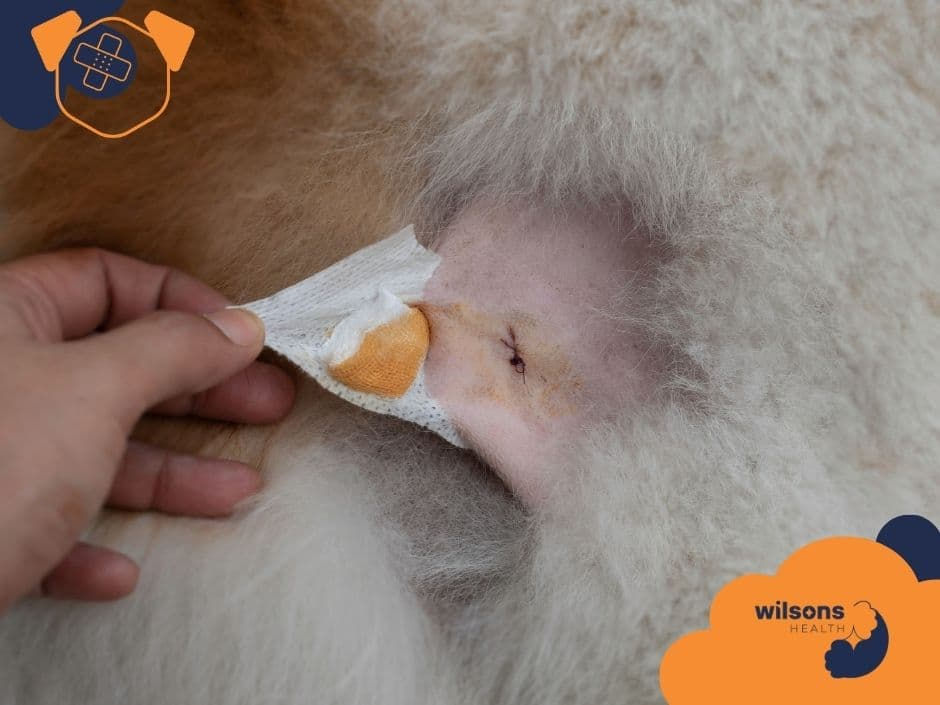
Under fur, a wound can look small while extending deep into tissue. A puncture from a tooth or stick may be barely visible – but carry bacteria into muscle, joints, or even the chest cavity. What looks like “a little nip” after a scuffle can be the starting point of an abscess days later.
This gap between what we see on the surface and what’s happening inside the body is exactly where uncertainty – and anxiety – lives for many dog owners. You don’t want to overreact, but you really don’t want to miss something important either.
This article is meant to sit in that space with you: to give you a clearer mental map of when a wound can reasonably be managed at home – and when it’s time to get professional eyes (and hands) on it.
First, a quick shared language: what counts as a “wound”?
Veterinary teams use a few basic terms that are helpful to know:
Open wound – Any break in the skin that exposes the underlying tissue. This ranges from a scraped belly to a deep bite.
Common wound types
Abrasion: surface scrape, like “road rash” or grass burn.
Laceration: a cut or tear with uneven edges (from glass, fences, claws).
Puncture: a small opening with a deeper track (most dog bites, sticks, nails).
Abscess: a pocket of pus under the skin, often from an old puncture or bite.
Chronic wound: a wound that just doesn’t heal properly or keeps reopening.
Debridement – The vet removes dead, damaged, or infected tissue to give healthy tissue a chance to heal.
Second-intention healing – Letting the wound heal “from the inside out” rather than stitching it closed, often used when a wound is contaminated or infected.
You don’t need to use these words with your vet, but recognizing them can make conversations feel less overwhelming – and more like a partnership.
The non-negotiable red flags: call your vet immediately
There are some situations where “wait and see” is not your friend. These are the times to call your vet (or an emergency clinic) right away.
1. Bleeding that doesn’t stop within about 10 minutes
If you’ve:
Applied firm, direct pressure with clean gauze or a cloth
Held that pressure continuously for up to 10 minutes
And the wound is still bleeding significantly
…this is an urgent situation and needs veterinary care as soon as possible.[5][9]
A vet can:
Identify and control bleeding from deeper vessels
Check for internal injury
Decide whether sutures or bandaging are needed
Even if the bleeding eventually slows, heavy blood loss is a medical problem in itself.
2. Any wound near eyes, chest, abdomen, or joints
Location matters as much as size.
Seek professional help promptly if the wound is:
Near the eyes – even tiny scratches can threaten vision
On the chest or abdomen – risk of penetrating into the chest cavity or belly
Over a joint (knee, elbow, hock, wrist) – punctures here can reach the joint space and cause serious infections
On paws – especially deep cuts between toes or nail bed injuries
These areas contain structures (eyes, organs, joints, tendons) that don’t tolerate infection well and may need imaging, flushing, or more advanced care.[1][3][7]
3. Deep, gaping, or heavily contaminated wounds
A wound needs veterinary assessment if:
You can see fat, muscle, or other tissue layers
The edges are pulled apart or you can slide a cotton swab or finger in
There’s gravel, glass, grass, or other debris embedded in it
It was caused by a bite, car accident, or other high-force trauma
These wounds often need:
Surgical cleaning and debridement
Possible suturing or partial closure
Drain placement if there’s a pocket where fluid will collect
Pain relief and antibiotics as appropriate[1][3][7]
Trying to rinse out a deeply contaminated wound at home usually isn’t enough – and can be very painful for the dog.
4. You suspect a foreign object is still in the wound
If you think something may still be inside (a thorn, stick fragment, glass shard, metal), do not try to dig it out yourself.
Signs might include:
A visible piece of material in the wound
A puncture from a known object (stick, nail, fence wire)
A dog that yelps or resists if you gently touch the area
Foreign material often needs removal under sedation or anesthesia, along with imaging to be sure nothing is left behind.[1][7] Leaving it in place can lead to abscesses, chronic drainage, or serious infections.
5. Any sign of infection – especially if it’s getting worse
Infection can turn a small, manageable wound into a much bigger medical problem. Call your vet if you notice:
Redness that is spreading or becoming more intense
Swelling around or under the wound
Heat compared to the surrounding skin
Discharge – especially yellow, green, or bloody fluid
Foul odor
Increased pain – your dog guards the area, growls, or won’t let you touch it
Your dog seems lethargic, loses appetite, or feels feverish to the touch[5][11]
These are classic signs that bacteria are winning the race against healing. Antibiotics, proper cleaning, and sometimes drainage are needed.[1][3][7]
6. Wounds that just won’t heal – or keep reopening
Most simple wounds start to look noticeably better within several days:
Less redness
Less swelling
A cleaner, drier surface
New tissue (a pink, bumpy “granulation” bed) starting to fill in
If instead you see:
A wound that looks the same (or worse) after several days
Tissue that looks gray, black, or dead
A wound that keeps breaking open or oozing
A sore that’s been there weeks without real progress
…this has moved into the territory of a chronic wound and needs a vet’s hands-on assessment.[3]
In these cases, your vet may:
Debride dead or infected tissue
Culture the wound to choose the right antibiotic
Change the dressing type
Consider advanced therapies like hydrogels, specialized bandages, or negative pressure wound therapy (NPWT) in more complex cases[3]
NPWT (a vacuum-assisted system) is promising but still an emerging area in veterinary medicine, with limited but encouraging clinical reports.[3]
7. Wounds from bites or fights – even if they “don’t look bad”
Dog bites are deceptive. Teeth act like needles: they push bacteria deep under the skin through small holes. The surface may close quickly, trapping contamination underneath.
Typical pattern:
Day 0: Minor puncture wounds, dog seems okay
Days 2–4: Swelling, warmth, and pain develop
Day 3–7: A soft, painful lump appears – an abscess full of pus
Veterinarians strongly recommend evaluation for any bite wound, especially if:
It’s from an unknown dog or wild animal (rabies risk, vaccination concerns)
Your dog is small and the other dog was large
The bite is near the chest, abdomen, neck, or joints
Your dog is already painful, limping, or lethargic[1][3][7]
Even if your dog “walked away from the fight,” internal trauma and infection risk are real. Early cleaning, possibly antibiotics, and monitoring can prevent abscess formation and more invasive procedures later.
8. Your dog is in obvious pain, shock, or distress
Regardless of what the wound looks like, seek urgent care if your dog:
Is very quiet, unresponsive, or collapses
Has pale gums
Is breathing rapidly or with effort
Cries, whimpers, or growls when touched anywhere
Can’t stand or walk normally
These signs suggest systemic impact – blood loss, internal injury, or shock – and go far beyond local wound care.[9][13]
Home care vs. vet care: where is the line?
A useful way to think about it:
You can safely manage minor, superficial wounds at home – but you cannot safely “guess” with deep, contaminated, or worsening wounds.
What’s usually reasonable for home care (after a quick vet check if you’re unsure)
Very superficial abrasions or scrapes
Small cuts that:
Are not deep
Are not over joints, eyes, or body cavities
Stop bleeding with <10 minutes of pressure
Have clean edges and no debris
For these, typical vet-backed guidance includes:
Direct pressure initially to stop bleeding[5][9]
Gentle cleaning with water or a pet-safe antiseptic solution, usually twice daily[1][5][11]
Preventing licking and chewing (Elizabethan collar or alternatives)
Importantly:Avoid using hydrogen peroxide, alcohol, or harsh disinfectants unless your vet specifically instructs otherwise. They can damage healthy tissue, delay healing, and cause pain.[1][5]
What almost always needs professional evaluation
Any of the red flags listed above
Wounds larger than a few centimeters
Puncture wounds from bites, sticks, or nails
Wounds in high-risk locations (eyes, chest, abdomen, joints, paws)
Wounds in dogs with other health issues (diabetes, immune disease, on steroids, very old or very young)
When in doubt, a quick phone call with your vet’s team can be clarifying. Describe:
Where the wound is
How it happened (if you know)
How much it bled
What it looks like now
How your dog is acting overall
You’re not “bothering” them; this is exactly what they’re there for.
What your vet might do (and why it matters)
Understanding what happens at the clinic can make the decision to go in feel less intimidating.
Depending on the wound, your vet may:
1. Assess the whole dog, not just the wound
They’ll check:
Heart rate, breathing, temperature
Gum color and hydration
Pain level and mobility
This helps rule out internal injuries or systemic infection that you can’t see from the outside.[9][13]
2. Clean and debride the wound properly
This may involve:
Clipping fur around the area
Flushing with large volumes of sterile fluid (volume matters more than the specific solution)[7]
Removing dead tissue (debridement) so healthy tissue can grow[1][3]
It’s not glamorous work, but it’s one of the biggest predictors of whether the wound will heal smoothly or turn into a chronic problem.
3. Decide: close it, partly close it, or leave it open
This is often where owners feel confused, because it can seem counterintuitive.
Clean, fresh wounds (e.g., a kitchen-knife-like laceration seen quickly) may be sutured closed.
Contaminated or infected wounds are often left partially or fully open to drain and heal by second intention.[1][3]
It can feel unsettling to bring your dog in and leave with a wound that’s not stitched shut. But leaving a dirty wound closed is like sealing bacteria into a warm, moist box – a recipe for abscesses and deeper infection.
This is one of the ethical and practical tensions vets manage daily:Cosmetically “neat” vs. biologically safe.[3]
4. Prescribe antibiotics – when they’re truly needed
Antibiotics may be:
Topical (applied to the wound)
Oral or injectable (for deeper or more serious infections)[1]
Key points:
They’re not automatically needed for every minor wound.
When prescribed, they must be given exactly as directed and for the full course, even if the wound looks better earlier.[1]
Stopping early or skipping doses doesn’t just risk your dog’s recovery; it also contributes to antibiotic resistance.
5. Provide pain relief and home-care instructions
Good wound care almost always includes pain management. A dog that’s comfortable:
Heals better (stress hormones drop, sleep improves)
Is easier to handle for bandage changes
Is less likely to develop fear around wound care
Vets will also give specific instructions on:
How often to clean or change dressings
What to watch for (signs of infection or delayed healing)
How to keep your dog from interfering with the wound (cones, clothing, activity limits)[1][5][7]
If anything is unclear, this is the moment to ask. Clear communication is not a luxury here; it directly improves healing and your peace of mind.
The emotional side: wounds don’t just happen to skin
Wounds from accidents, fights, or bites aren’t only physical. They can carry emotional and psychological weight – for both dogs and humans.
For dogs
Traumatic injuries can lead to:
Anxiety or fear around other dogs, certain places, or handling
Startle responses, hypervigilance, or avoidance
Signs that look like PTSD in humans – while the exact parallels are still being studied, many dogs clearly show trauma-related behavior changes[2][8][10]
Painful or chronic wounds can also:
Make dogs grumpy or irritable
Reduce playfulness
Trigger defensive behaviors if someone goes near the sore area
Behavioral support, gentle handling, and – in some cases – behavioral meds or supplements under veterinary guidance can help.[2][10][16]
For owners
The emotional load is often underestimated:
Guilt (“If I’d noticed sooner…”, “I should have prevented that fight”)
Anxiety about making mistakes with wound care
Stress over costs, time, and the sight/smell of the wound itself
Sleep disruption from nighttime checks or worrying
This emotional burden can actually affect how consistently wound care is done – an area researchers are still exploring.[3] The more supported and informed you feel, the easier it is to stick with the plan.
It’s okay to:
Tell your vet that the wound grosses you out or scares you
Ask for a demonstration the first time they show you how to clean or bandage it
Admit if the schedule they propose doesn’t feel realistic for your life
Most veterinary teams would rather adjust a plan than watch a perfect-on-paper plan quietly fall apart at home.
Creating a healing environment at home
Beyond the bandages and medications, the environment your dog recovers in matters.
Research and clinical experience suggest that:
Calm, predictable routines support both physical healing and emotional recovery[6]
A safe, quiet resting area away from household chaos can lower stress
Gentle touch, soothing voice, and low-stress handling techniques reduce fear during wound care[16]
For some dogs, complementary therapies like acupuncture, massage, or hydrotherapy may help comfort and mobility, when integrated into a vet-guided plan[6]
Evidence for many complementary approaches is still emerging, and long-term effects aren’t fully understood.[3][6] The key is that they should support, not replace, proper medical wound management.
A simple decision guide you can keep in your head
When you notice a wound, you can mentally run through four quick questions:
How bad is the bleeding?
Stops with pressure within ~10 minutes → monitor
Does not stop / is heavy → vet now
How deep / where is it?
Superficial, small, not over high-risk areas → may be home-manageable
Deep, gaping, near eyes/chest/abdomen/joints/paws → vet
How dirty or complicated is it?
Clean, recent, no debris → basic cleaning may be enough
Debris, bite wounds, suspected foreign object, or major trauma → vet
What’s happening over time?
Looks better day by day → keep going as advised
Looks worse, smells, swells, or stalls → vet
If at any step you feel uneasy or something doesn’t match what you expected, that in itself is a valid reason to call.
It’s not your job to be certain
One of the quiet pressures many dog owners feel is the sense that they should know whether something is “serious enough” before involving a professional.
The reality:
Wounds are often biologically more complex than they appear.
Even experienced vets use imaging, sedation, and time to fully understand them.
Your job is not to be certain; your job is to notice, respond, and ask.
If you bring in a wound that turns out to be minor, you haven’t “wasted” anyone’s time. You’ve bought yourself reassurance, and you’ve given your dog the benefit of professional eyes on a vulnerable moment.
And if you bring in a wound that needed help, you’ve done something quietly profound: you’ve shortened suffering, reduced risk, and made healing more likely – physically and emotionally.
That’s not overreacting. That’s caregiving.
References
VCA Canada Animal Hospitals – Care of Open Wounds in Dogs.
PetCareRx – Emotional Scars Healing for Dogs.
Pavletic, M.M. et al. Principles of wound management and wound healing in veterinary medicine. PMC.
My Pacific Health – Dogs Aid Recovery from Trauma and Grief.
Pittsboro Animal Hospital – Dog Wound Care Guide.
Animal Wellness Magazine – Complementary Treatments for Trauma in Dogs.
Today's Veterinary Practice – Wound Management in Veterinary Patients.
Talented Ladies Club – Emotional Impact of Dog Fight Injuries.
NCBI Bookshelf – EMS Canine Wound Care.
PetMD – Healing Emotionally Traumatized Pets.
Southgate Animal Hospital – Dog Wound Care.
South Texas Law Firm – Emotional Impact of Dog Bite Accidents.
Allogy – K9 Clinical Practice Guideline #14 Wound Management.
Psychology Today – Animals and Attachment Trauma Healing.
Air Force News – Dogs Assist Wounded Airmen Recovery.
Veterinary Nurse Journal – Low-Stress Handling for Long-Term Wound Care.






Comments